Erythematotelangiectatic Rosacea (ETR): Symptoms, Triggers & Treatment
When patients come to us worried about persistent facial redness, one of the most common diagnoses we make is erythematotelangiectatic rosacea, often shortened to ETR. This type of rosacea leads to ongoing flushing, visible tiny blood vessels and a burning or stinging sensation across the central face, which many people initially mistake for sensitive skin or sun damage. As consultant dermatologists, we see first-hand how much this can affect confidence, especially when redness flares at work, social events or seemingly for no reason at all.
At our Dermatology clinic in London, we see the full spectrum of rosacea, from mild flushing to more advanced forms, and ETR is frequently the starting point. The positive news is that with the right diagnosis, a clear understanding of your triggers and a tailored treatment plan, we can usually bring symptoms under much better control. Our role is to guide you through what ETR is, why it happens, and which combination of skincare, lifestyle and medical treatments is most likely to help your skin feel calmer and look more even day to day.
Because we manage rosacea every week in clinic, we draw on both our clinical experience and the latest evidence when advising on treatment options. We also understand that no two patients are the same; some are mainly troubled by flushing, others by fixed redness and fine vessels, and many by the discomfort and heat that accompany their symptoms. Our aim is always to combine effective medical care with practical, realistic advice you can live with.
What Is Erythematotelangiectatic Rosacea?
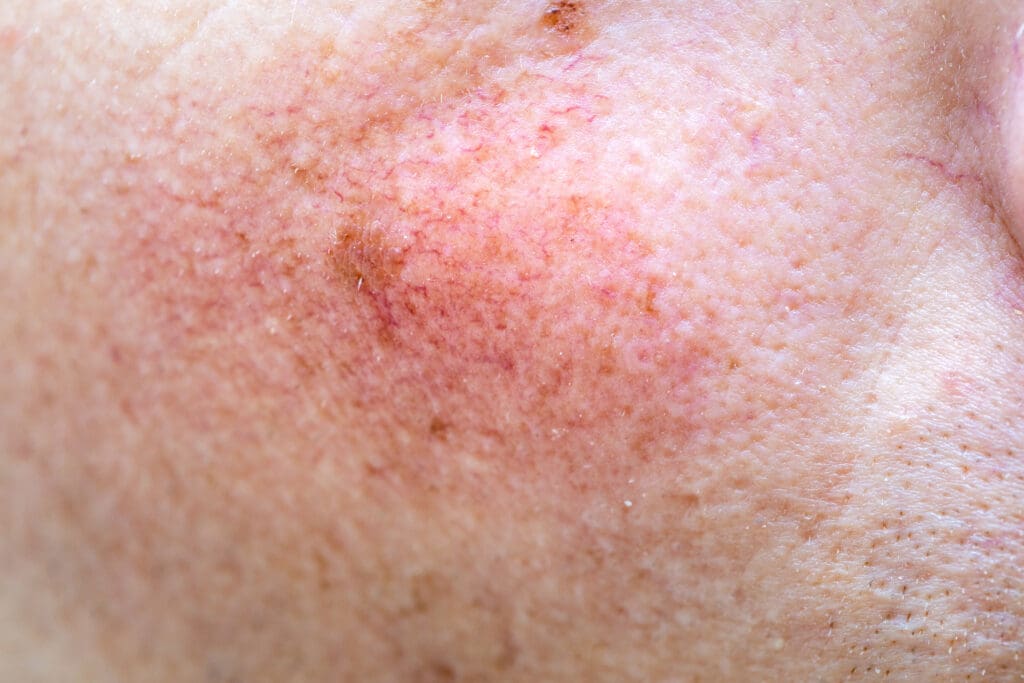
Erythematotelangiectatic rosacea is the vascular subtype of rosacea, characterised by frequent flushing, persistent redness across the central face and visible small blood vessels called telangiectasias. It typically affects the cheeks, nose, forehead and sometimes the chin, while the skin around the eyes is often spared. People with ETR often describe their skin as feeling hot, sensitive or “on fire”, particularly during a flare.
From a clinical perspective, we see ETR as a chronic, relapsing condition, which means symptoms tend to come and go over time rather than clearing completely. Without treatment, flushing episodes can gradually progress to more persistent background redness and more prominent visible vessels. Many patients also notice that their skin reacts strongly to skincare products, water temperature and even minor weather changes, which can make everyday routines more challenging.
At our clinic we provide consultant‑led rosacea specialist treatments as part of our wider medical dermatology services, so we can distinguish ETR from other causes of facial redness such as dermatitis, lupus or contact allergy. Getting the diagnosis right is crucial, as the best treatment strategy for ETR will differ from that used for acne‑type or phymatous rosacea.

Common Symptoms of ETR
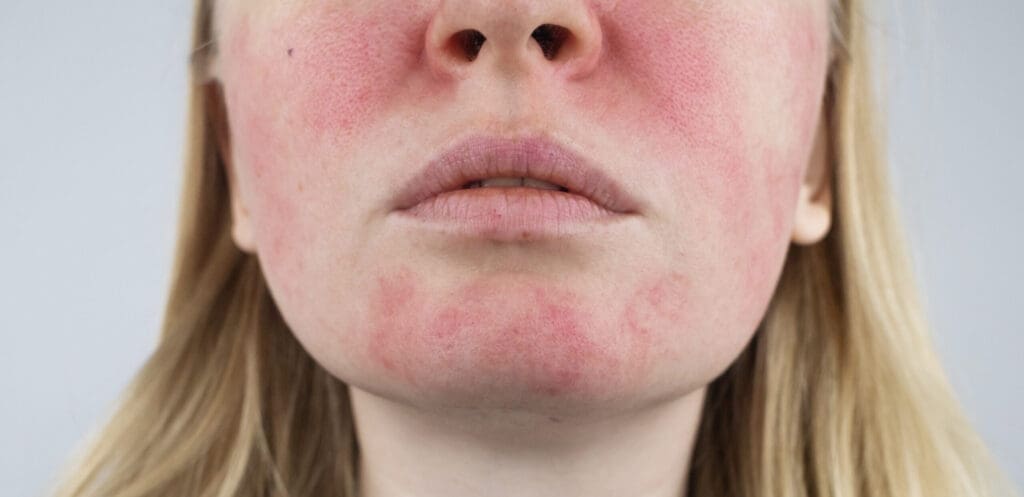
While every person’s experience is slightly different, there are several hallmark symptoms of erythematotelangiectatic rosacea that we look for in clinic. These include:
- Persistent facial redness across the cheeks, nose, forehead and sometimes chin.
- Frequent flushing or blushing episodes that last longer than usual.
- Visible thread‑like blood vessels close to the skin’s surface (telangiectasias).
- Burning, stinging or heat in the affected areas, especially when applying skincare.
- Increased sensitivity, dryness or fine scaling over the red areas.
Many patients tell us that their skin feels uncomfortable or painful rather than just red, which can affect sleep, exercise and social confidence. Over time, if ETR is left untreated, flares may become more frequent and the baseline redness more permanent, which is why early assessment can make such a difference. Our consultant‑led rosacea treatment pathway is designed to assess these symptoms carefully and build a treatment plan tailored to your particular pattern of redness and discomfort.
What Causes ETR and What Triggers Flares?
The exact cause of erythematotelangiectatic rosacea is still being studied, but evidence points to a combination of abnormal blood vessel responses, immune system changes and nerve sensitivity in the skin. In ETR, the facial blood vessels tend to dilate too easily and stay open for longer than they should, leading to repeated flushing and eventually fixed redness. Researchers have also identified changes in inflammatory pathways and nerve signalling, which may help explain the burning and stinging sensations many patients describe.
On top of this underlying tendency, a wide range of everyday factors can trigger ETR flares. Common triggers include heat, hot showers, sun exposure, wind and temperature extremes; hot drinks, spicy foods and alcohol; emotional stress; and vigorous exercise, especially in a warm environment. Certain skincare products, fragranced cosmetics and topical steroids can further irritate the skin and worsen redness.
During your consultation with us, we spend time going through your history to identify which triggers are most relevant for you personally. This often includes discussion of hormones, lifestyle, workplace environment and previous treatments you’ve tried. We then help you put together a practical trigger‑minimising plan alongside medical treatment, drawing on guidance from trusted UK resources such as Patient.info and NHS‑aligned recommendations on rosacea management.
How We Diagnose Erythematotelangiectatic Rosacea
A clear diagnosis is the first step towards effective control. At our Harley Street clinic, all rosacea assessments are carried out by consultant dermatologists with extensive experience in recognising the different subtypes of rosacea. We start by listening carefully to your symptoms – when the redness started, how it behaves, how it feels, and how it affects your day‑to‑day life.
We then examine the skin closely to assess the pattern and severity of redness, the presence of telangiectasias and any associated features such as eye symptoms or acne‑like bumps. In most cases, we can diagnose ETR based on your history and clinical examination alone, without the need for invasive tests. Where there is diagnostic uncertainty, or if we suspect another condition is contributing, we may perform additional tests or work with other specialists.
Our rosacea specialist treatments are delivered within a comprehensive medical dermatology service, which means we can also address any related skin issues such as seborrhoeic dermatitis or acne that may be complicating your picture. We know from experience that understanding your condition clearly can be just as important as the treatment itself in helping you regain a sense of control.
Treatment Options for Erythematotelangiectatic Rosacea
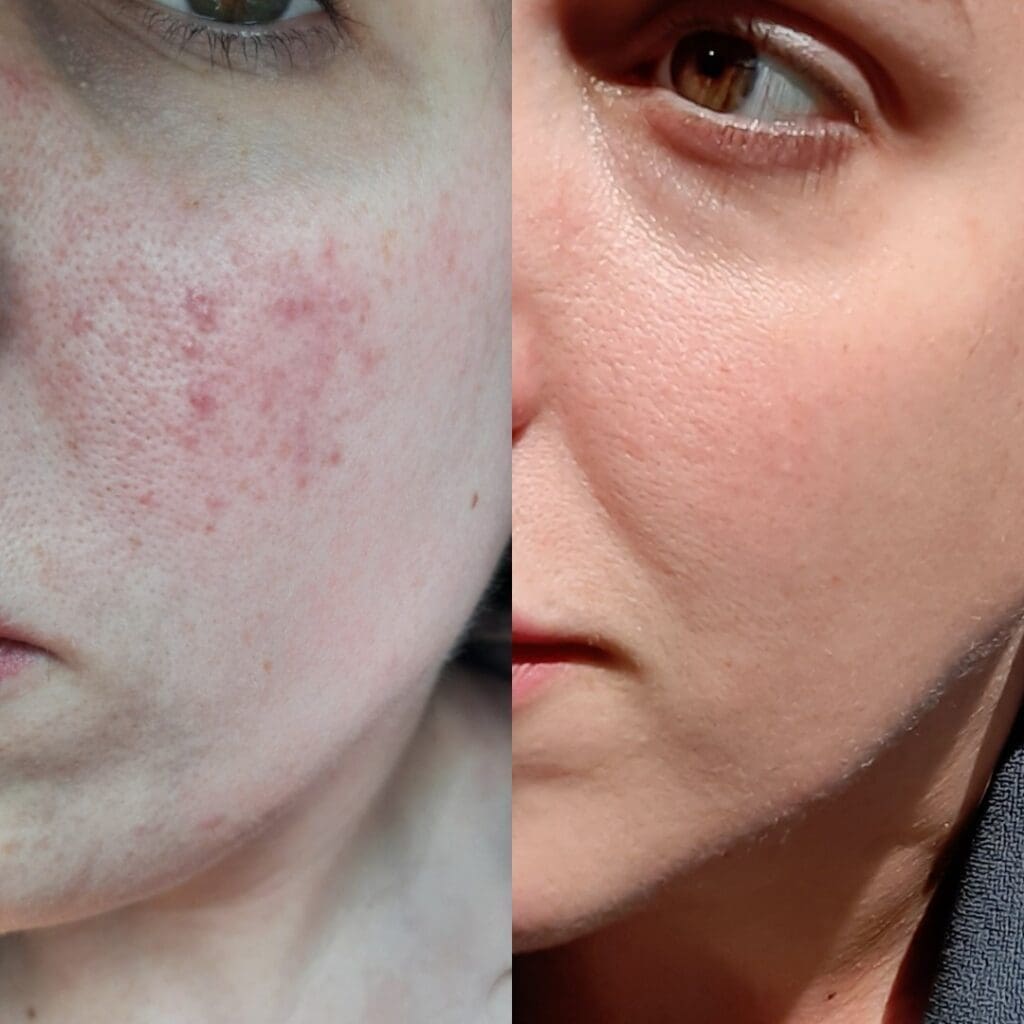
There is no single cure for ETR, but there are many effective ways to reduce redness, improve comfort and minimise flares. In practice, treatment usually involves a combination of gentle skincare, lifestyle measures, targeted prescription medication and, in many cases, laser or light‑based therapies.
At our Harley Street clinic, we begin by optimising your skincare routine: using non‑irritating cleansers, fragrance‑free moisturisers and daily high‑factor sun protection, all of which help support the skin barrier and reduce sensitivity. We will then discuss medical treatments tailored to your symptoms, which may include topical agents to reduce redness and oral medication for more severe or persistent flushing. For many patients with ETR, laser and light treatments play a central role in visibly reducing background redness and broken vessels, and we are able to offer these in‑house as part of our skin rejuvenation and rosacea programmes.
We also draw on our own guidance on different rosacea subtypes to choose the right combination of treatments for you, integrating medical care with appropriate cosmetic dermatology options where beneficial. We always balance potential benefits with downtime, comfort and cost so that your treatment plan is realistic and sustainable for you.
Laser and Light-Based Treatments for Facial Redness
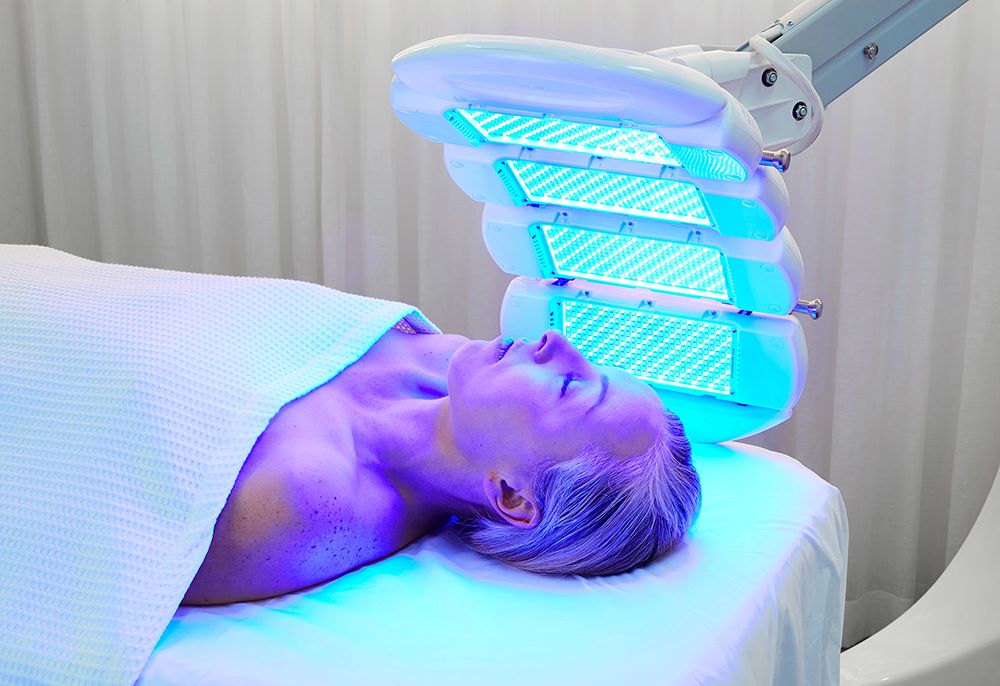
Laser and light‑based therapies are often particularly helpful in erythematotelangiectatic rosacea, where visible vessels and diffuse redness are prominent. These treatments work by targeting excess blood in the superficial vessels, causing them to collapse and gradually be reabsorbed by the body, which in turn reduces redness and the appearance of small veins.
At our clinic, we commonly recommend Intense Pulsed Light (IPL) or vascular‑targeting lasers as part of a structured plan for persistent facial redness. IPL is especially useful for diffuse redness and fine telangiectasias, while fractional laser can be helpful where there is associated texture change or sun damage. Most patients need a course of several sessions, spaced a few weeks apart, and many report not only visible improvement but also better comfort and fewer severe flares.
These technologies sit alongside our other skin rejuvenation techniques, allowing us to tackle redness, texture and pigmentation together where needed. As with all procedures, treatments are delivered or supervised by consultant dermatologists to help ensure safety and effectiveness.
Living With ETR: Self-Care and When to Seek Help
Living with erythematotelangiectatic rosacea can be challenging, but small, consistent changes often make a big difference over time. We generally recommend keeping a trigger diary, protecting your skin from the sun daily, avoiding harsh skincare and being cautious with very hot environments, including saunas and hot yoga. Choosing gentle, fragrance‑free products and avoiding over‑exfoliation helps to maintain the skin barrier, which is often compromised in ETR.
You should consider seeing a dermatologist if your redness is persistent, if flushing is affecting your quality of life or if over‑the‑counter products are making your skin feel worse rather than better. Our consultant‑led rosacea treatments service is designed for exactly this situation, providing rapid access to experienced specialists who can assess your symptoms and discuss all the available options with you. Early, tailored treatment can slow the progression of ETR, reduce the frequency and severity of flares, and help you feel more comfortable in your own skin again.
FAQs
Is erythematotelangiectatic rosacea the same as sensitive skin?
No. While the skin often feels very sensitive in ETR, it is a specific subtype of rosacea involving abnormal blood vessel responses and inflammation, rather than simple sensitivity alone.
Can ETR be cured?
ETR is a chronic condition, so we do not talk about a cure, but with the right combination of skincare, trigger management, medical treatment and laser therapy, most patients see significant, long‑term improvement.
Which treatments work best for persistent redness and visible veins?
Topical redness‑reducing treatments, in combination with laser or light‑based therapies such as IPL and vascular lasers, have strong evidence for improving background redness and telangiectasias in ETR.
Do you treat all types of rosacea at the clinic?
Yes. We provide comprehensive care for all forms of rosacea, including erythematotelangiectatic, acne‑type and ocular rosacea, through our dedicated rosacea specialist treatments service in Harley Street.
How can I arrange an appointment for my rosacea?
You can get in touch with us directly to arrange a consultation under our medical dermatology services; a consultant dermatologist will assess your skin, confirm the type of rosacea you have and create a personalised treatment plan.